Get A Testing Quote
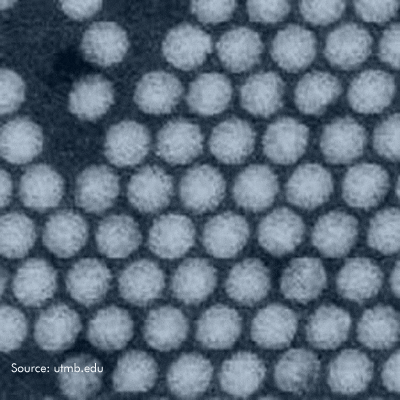
Poliovirus
| Virus | Poliovirus |
| Structure | Non-enveloped |
| Family | Picornaviridae |
| Host(s) | Humans |
| Disease(s) Caused | Several manifestations, ranging from mild to life-threatening |
| Symptoms | Fever, headache, stiffness/pain in the back or neck, muscle spasms/tenderness |
| Potential Complications |
Acute poliomyelitis: Flaccid paralysis, loss of reflexes Postpoliomyelitis Syndrome (PPS): Reoccurence of symptoms years after stabilization of acute symptoms |
| Transmission Mode |
Close person-to-person contact, contaminated fomitesFecal-oral, person-to-person contact, water, contaminated fomites |
| Sites of Community Outbreaks | Sewage-contaminated drinking water, poorly sanitized living areas with an unvaccinated population |
Importance of Poliovirus
The polioviruses are the most well-known members of the genus Enterovirus which also includes the echoviruses and Coxsackieviruses. Although poliovirus-related illnesses are believed to have been endemic in various human populations for well over a millennium, the widespread outbreaks most associated with the virus in the United States began during the mid-20th century. Prior to the advent of municipal-level water treatment and thus, readily-available potable water, infants were exposed to wild type polioviruses while still protected by maternal antibodies that provided an initial innate immunity. Repeated environmental exposure(s) further bolstered the host immune response over a lifetime. This natural process of human immunization was interrupted by water treatment, which effectively removed polioviruses and other pathogens of concern from drinking water. The resulting decrease in early childhood exposure led to a surge of susceptible adolescents who were infected during the peak of the pre-vaccine poliomyelitis outbreaks in the U.S. from 1950 to1955. Tens of thousands of children were permanently crippled by polio and several thousand died due to paralysis of the muscles required for breathing. The killed- and live-virus vaccines developments subsequently spearheaded by Jonas Salk and Albert Sabin, respectively, despite their own unique pros and cons, eventually led to eradication of polioviruses from the U.S. in the late 1970s. However, outbreaks of poliomyelitis continue to be recorded around the world in sub-populations of unvaccinated persons (10, 12, 13), with increasing numbers traced to vaccine-derived poliovirus strains in developing countries (9). Therefore, the worldwide eradication of poliovirus remains a top priority for the World Health Organization and a number of aid groups.
There are three known serotypes of poliovirus (PV1, PV2, and PV3) – each are known to only infect humans, with PV1 the most commonly isolated during epidemics (5). Each of the serotypes has a slightly different capsid protein composition; therefore, infection with one serotype does not necessarily impart immunity to the other two serotypes (4). Transmission of polioviruses is by the fecal-oral route similar to the other enteroviruses. Replication initiates in the pharynx and gastrointestinal tract, and the vast majority of infected persons are asymptomatic. Following a transient viremia (virus present in the blood), there is a small chance [<2% (16)] of the virus then invading the central nervous system where motor neurons are subsequently infected, leading to the neurological symptoms associated with poliomyelitis (e.g. flaccid paralysis). Of those cases, there is 5-10% mortality rate due to paralysis of the respiratory muscles. Whether the resulting illness is mild or life-threatening, viruses are shed in the stool for several weeks, resulting in a continuous source of infectious viruses in the environment.
Environmental Viability of Polioviruses and Importance of Disinfection
Polioviruses are characterized by a non-enveloped, nucleocapsid structure, and can remain viable on porous (e.g. paper and cotton cloth) and nonporous surfaces (e.g. glazed tile and aluminum) for up to 30 days with no clear correlation between viability and the presence of organic matter (2). Polioviruses are also more subject to inactivation during the process of desiccation relative to other enteric viruses such as hepatitis A (1). Thus, they are of concern chiefly in the area of water quality due to historical epidemiological aspects (i.e. both waterborne and direct transmission routes). In addition, polioviruses maintain high titer levels and infectivity in aqueous environments, with greater survivability in drinking water and freshwater relative to seawater (6, 8). However, a number of water treatment processes have proven to effectively inactivate polioviruses, including both natural and anthropogenic sources of UV radiation (7, 11) and ozone (15).
For disinfection efficacy evaluations, polioviruses are largely employed as model non-enveloped viruses for suspension-based studies. A recent evaluation of natural and commercially-available disinfectants found that of nine products, only two (which were sodium hypochlorite- or QAC-based) demonstrated a ≥3-log10 reduction of polioviruses in the absence of an organic soil load at 30 seconds and 5 minutes (14). A separate study comparing the susceptibility of polioviruses in the presence of organic soil (20% feces) relative to 0% soil (PBS-only) confirmed the efficacy of sodium hypochlorite in addition to diethylenetriamine. No correlation was found between the presence of organics and viral persistence in suspension, although surface studies may generate different data (1). Further work has demonstrated the anti-viral efficacy of low levels (<2%) of glutaraldehyde against poliovirus in the disinfection of digestive endoscopes used in hospitals and other healthcare settings (3).
References
- Abad, F., R. Pinto, and A. Bosch. 2006. Disinfection of human enteric viruses on fomites. FEMS Microbiology Letters. 156: 107-111.
- Abad, F., R. Pinto, and A. Bosch. 1994. Survival of enteric viruses on environmental fomites. Applied and Environmental Microbiology. 60: 3704-3710.
- Bailly, J. et al. 1991. Activity of glutaraldehyde at low concentrations (less than 2%) against poliovirus and its relevance to gastrointestinal endoscope disinfection procedures. Applied and Environmental Microbiology. 57: 1156-1160.
- Centers for Disease Control and Prevention. Poliomyelitis: Epidemiology and Prevention of Vaccine-Preventable Diseases. The Pink Book: Course Textbook – 12th Edition Second Printing, May 2012.
- Chumakov, K. et al. 2007. Vaccination against polio should not be stopped. Nature Reviews Microbiology. Advance Online Publication, published online 29 October 2007; doi:10.1038/nrmicro1769.
- Enriquez, C., C. Hurst and C. Gerba. 1995. Survival of enteric adenoviruses 40 and 41 in tap, sea, and waste water. Water Research. 29: 2548-2553.
- Heaselgrave, W. et al. 2006. Solar disinfection of poliovirus and Acanthamoeba polyphaga cysts in water – a laboratory study using simulated sunlight. Letters in Applied Microbiology. 43: 125-130.
- Hurst, C., W. Benton, and A. McClellan. 1989. Thermal and water source effects upon the stability of enteroviruses in surface freshwaters. Canadian Journal of Microbiology. 35: 474-480.
- Kew, O. et al. 2004. Circulating vaccine-derived polioviruses: current state of knowledge. Bulletin of the World Health Organization. 82: 16-23. Kim-Farley, R. et al. 1984. Outbreak of paralytic poliomyelitis, Taiwan. The Lancet. 324: 1322-1324.
- Meng, Q.S. and C. Gerba. 1996. Comparative inactivation of enteric adenoviruses, poliovirus and coliphages by ultraviolet irradiation. Water Research. 30: 2665-2668.
- Oostvogel, P. et al. 1994. Poliomyelitis outbreak in an unvaccinated community in the Netherlands. The Lancet. 344: 665-670.
- Poyry, T., M. Stenvik and T. Hovi. 1988. Viruses in sewage waters during and after a poliomyelitis outbreak and subsequent nationwide oral poliovirus vaccination campaign in Finland. Applied Environmental Microbiology. 54: 371-374.
- Rutala, W. et al. 2000. Antimicrobial activity of home disinfectants and natural products against potential human pathogens. Infection Control and Hospital Epidemiology. 21: 33-38.
- Shin, G-A. and M. Sobsey. 2003. Reduction of Norwalk virus, poliovirus 1, and bacteriophage MS2 by ozone disinfection of water. Applied Environmental Microbiology. 69: 3975-3978.
- Strauss, J.H. and E.G. Strauss. Viruses and Human Disease. Elsevier Academic Press, Burlington, MA. 2008.
Share

